| Home . About IRIS . Early Intervention . Clinical Guidelines . Tool Kit . Service Development . E.I Services . Research & Development . Training Courses . Questions & Answers . Links |
| Return to Early Intervention Services |
The Birmingham Early Intervention Service - Organisational Background
The Birmingham Early Intervention Service (EIS), part of the Northern Birmingham Mental Health NHS Trust, commenced in 1990 and developed to become community based in 1995. The service provides treatment and support to young people from different racial and cultural backgrounds living in the inner-city during the early years of psychosis from the first psychotic episode. These young people are often at critical transition points in their lives i.e. finishing education, starting employment, moving from home and starting long-term relationships. The EIS provides comprehensive care for 3 years.
Principles
The EIS provides specialist care for individuals who are in the early phase of psychosis using a team Assertive Outreach model of care. The service supports the notion that intervention within the "critical period" will promote optimum early symptomatic, social and personal recovery. The IRIS (Initiative to Reduce the Impact of Schizophrenia) principles and guidelines are reflected within clinical practice. Interventions are formulated and tailored so that gender, ethnicity and individual variations in recovery style are taken into account.
Aims and goals of the Early Intervention Service
- Early identification and treatment of psychosis
- Promotion of early recovery
- Minimisation of residual primary and secondary symptoms and relapse
- Provide youth friendly services emphasising social roles
- Support family and friends
- Promote personal control over psychosis
Evidence based practice is provided to clients including a low dose neuroleptic medication regime, cognitive therapy for hallucinations and delusions and specific psychosocial interventions for personal and social recovery. These interventions place great emphasis on the establishment of appropriately valued roles and goals and promoting self-management techniques.
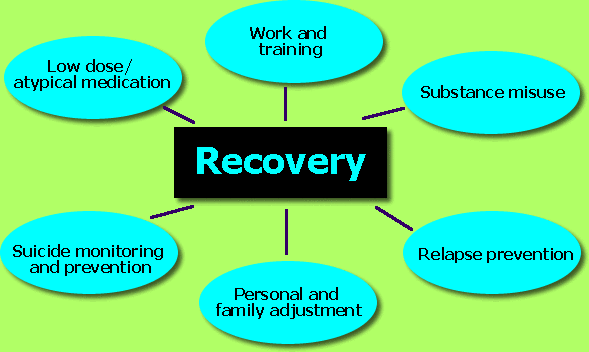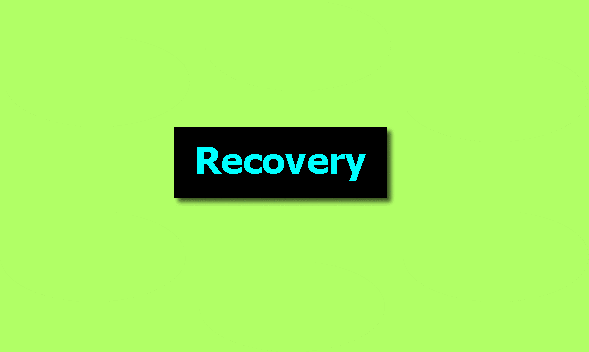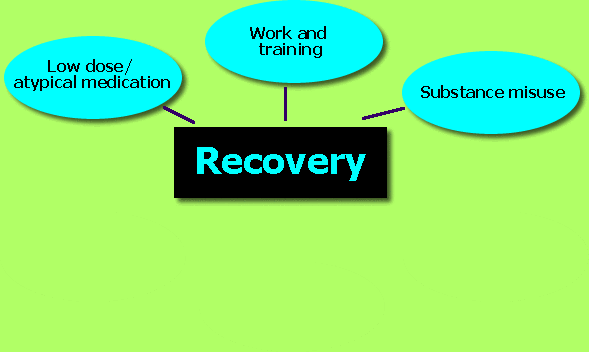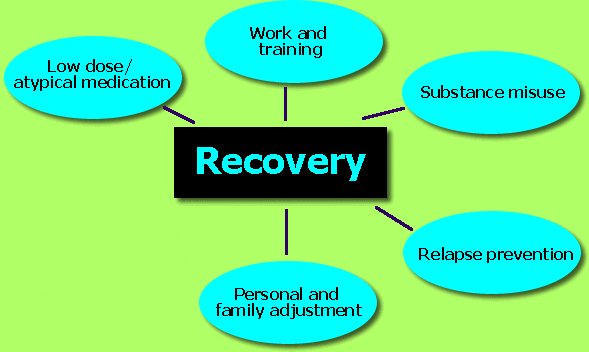
Structure of the Early Intervention Service
The EIS operates on the basis of mobile intensive interventions, seven days a week accessible service, and a single point of contact for referrers, users and carers through a keyworker.
Clients are usually referred to the EIS through a GP, psychiatric emergency teams or a primary care liaison service. Selection criteria include age (16-30), inner-city residency and evidence of hallucinations, delusions, thought disorder or gross behavioural disturbance indicative of psychosis. Clients should have had no prior lengthy contact with psychiatric services and the onset of symptoms fall within the critical period. Initial screening and assessment is provided by members of a multi-disciplinary intake team.
Once accepted by the service, each client meets a keyworker who takes responsibility for engagement and co-ordinating care via the Care Programme Approach (CPA). Interventions are operated through five clinical programmes:- vocational and pre-vocational training; cognitive therapy; recovery; social recovery and family intervention.
A weekly meeting takes place for supervision, review and training purposes and discuss the progress of clients.
Respite and Recovery unit
The EIS has a respite and recovery unit which is available to those requiring additional help and support during their recovery period. Residents are usually those who are struggling to manage in community settings and therefore the unit serves as a respite to avoid full admission to hospital. The unit works as a social recovery team and aims to improve the clients' interpersonal functioning and daily living skills. Close links between the client's keyworker and the team on the unit are maintained at all times.
Staffing
- The Service Director is responsible for strategic development of the service.
- Operational management is provided by an outreach team leader and a respite facilities manager.
- Medical: Consultant psychiatrist (3 sessions per week), clinical specialist ( 4 sessions per week), SCMO full time.
- Psychology: Consultant clinical psychologist (full time), research psychologist, 2 psychology assistants
- Nursing: 8 Community Psychiatric Nurses, 6 RMNs, 6 support workers
- Occupational Therapy: Senior I OT, OT technician
- Social Worker: 1 full time
- Administration: Business manager, 2 secretaries
Research and Development
The EIS realises the importance of Research and Development and the need to constantly re-evaluate its intervention protocol. Pathways to care and the amount of time every new referral has suffered his/her untreated psychosis are monitored. Other measures of symptomatic and social recovery are measured at acceptance to the service and annually and kept on a database. These include PANNS, Quality of Life Scale, Calgory Depression Scale, relapse, suicidal thinking and behaviour. Numerous publications from members of the EIS team can be found in books and journals on early intervention and psychological management of psychosis.
Exit
Exit from the service is planned throughout the time clients are with the EIS with a particular focus in the final year. Contact with GPs is made within the first six weeks and maintained throughout. Clients leaving the service receive the minimum aoptimum support to facilitate independence. Some clients are discharged back to primary care, others receive input from respite and recovery teams. Clients with complex continuing needs are managed by an area Assertive Outreach team. Occasionally clients stay for a little longer than 3 years if there are specific treatments only partially completed or until a crisis can be resolved.
Beacon status
The EIS became a NHS beacon service in 1999 which has increased the ability to disseminate the practice and research generated from the service. As well as offering beacon site visit days, the service mentors other trusts setting up early intervention teams and offers clinical placements to staff wishing to spend a few weeks working within the team. The EIS hosts the regional IRIS meetings and team members are actively involved with this group
| Return to the top of the page |
| Home . About IRIS . Early Intervention . Clinical Guidelines . Tool Kit . Service Development . E.I Services . Research & Development . Training Courses . Questions & Answers . Links |